Basal Cell Carcinoma (BCC)

What is a basal cell carcinoma (BCC)?
A basal cell carcinoma (BCC) is a type of skin cancer. There are two main types of cancer that affect the skin:
- melanoma and
- non-melanoma skin cancer
BCCs are a type of non-melanoma skin cancer. BCCs are the most common type (greater than 80%) of all skin cancer in the UK. BCCs are sometimes referred to as ‘rodent ulcers’.
Dr Hussain is an expert in the treatment of BCC and is Chair of the Regional Skin Cancer Multi-Disciplinary Team.
What causes basal cell carcinoma (BCC)?
Exposure to ultraviolet (UV) light from the sun or from sunbeds is the commonest cause of BCCs. Although BCCs may occur anywhere on the skin, they are most common on areas that are exposed to the sun (face, head, neck and ears). It is also possible for BCCs to develop in a longstanding scar.
Are you at risk of developing a basal cell carcinoma (BCC)?
Those with the highest risk of developing a basal cell carcinoma are:
- People with pale skin who burn easily and rarely tan
- Those who have had a lot of exposure to the sun (those with outdoor hobbies or outdoor workers and people who have lived abroad in warm climates)
- People who have used sun beds or have regularly sunbathed.
- People who have previously had a basal cell carcinoma.
Can basal cell carcinomas (BCCs) run in families?
There is a rare condition called Gorlin’s syndrome in which BCCs do run in the family. As a general rule however, BCCs are not hereditary. However some of the things that increase your risk of getting a BCC such as your skin type & how easily you burn for example does run in families.
What do basal cell carcinomas (BCCs) look like?
BCCs vary greatly in their appearance and it is therefore important to ensure a skin cancer expert assesses your skin at the earliest opportunity. If you have a scab that bleeds and does not heal completely or a new lump on the skin seek advice from a specialist. Some BCCs are superficial (in the top layer of the skin with no ‘roots’) and look like a scaly red patch on the skin and may often be misdiagnosed as eczema or dermatitis. Other BCCs form a lump and have a pearly edge surrounding a central crater. Often small red blood vessels are visible across the surface. Pain is not a usual feature of BCCs, although sometimes they can be itchy & bleed if caught. If left untreated, BCCs will eat away at the skin like a ‘rodent’ and eventually lead to a non-healing ulcer, thus giving rise to the term ‘rodent ulcer’. Some BCCs on the face are considered high-risk and so it is important to seek advice and guidance as soon as possible.
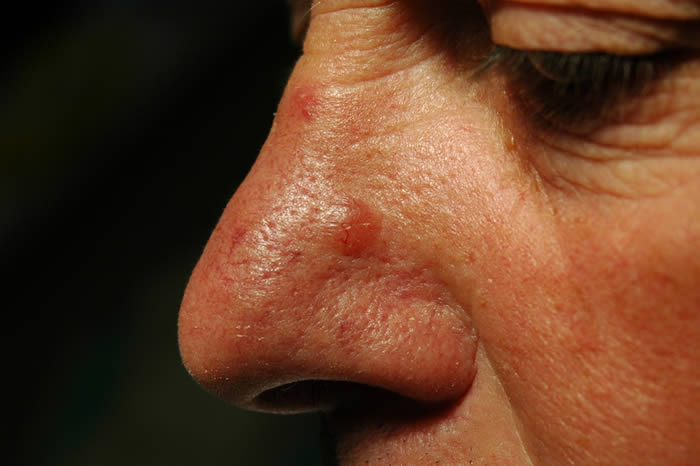
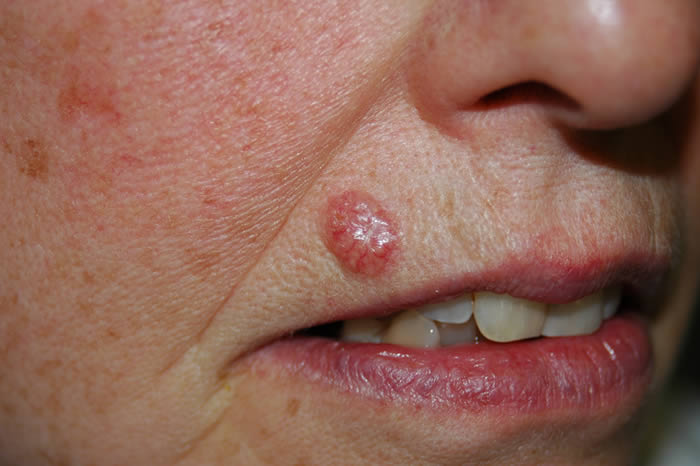
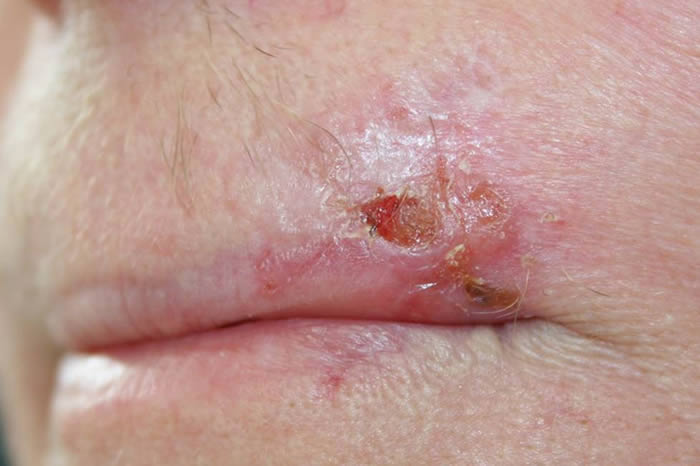
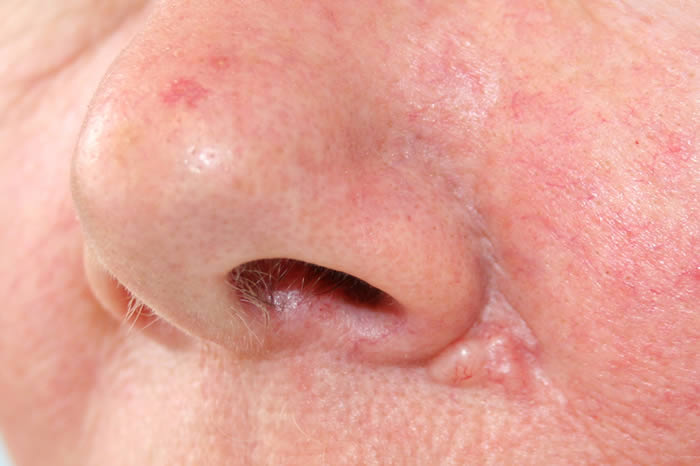
How will my basal cell carcinoma (BCC) be diagnosed?
Dr Hussain’s specialist expertise often allows him to make the diagnosis of a BCC just be examining your skin with magnification and good lighting. Sometimes, taking a sample in the form of a small skin biopsy can be performed under a local anaesthetic to confirm the diagnosis.
Can basal cell carcinomas (BCCs) be cured?
As BCCs stay localised to the skin, if treated adequately by a trained specialist they can be cured in almost every case. However the treatment can be more complicated if the BCC has been present for a long time, or if it occurs in a high-risk site such as close to the eye or on the nose or ear.
How can a basal cell carcinoma (BCC) be treated?
Dr Hussain is an internationally recognised expert in the treatment of BCCs and will advise you on the best form of treatment in your particular case.
The commonest method of treating BCCs is to remove them with surgery performed under local anaesthesia (your skin will be asleep but you will be awake). The hole that is left after removing the BCC can then reconstructed in a number of ways including pulling the skin edges back together (primary repair), moving some skin around (skin flap) or attaching a patch of skin from elsewhere (skin graft). Dr Hussain will discuss with you which option he feels will give you the best possible cosmetic outcome.
Other treatment methods include:
If you have any questions or comments, or if you want to learn more about the services of Dr Walayat Hussain, please call 0113 388 2234 or submit an online form by clicking here.

